|
|
|
Late revenge of analogue insulins among T1D-patients?
I am concerned: B.Teupe, Bad Mergentheim, Germany |
Artikel als PDF
(PDF 178 KB)
|
To the Editor – Background
This data analysis was provoked by the plight of a young patient: 1999 type-1-diabetes became
manifest in a girl born 1992. Starting with ICT: Actrapid® / Protaphane®, 1 year later additional
Humalog®, since 2 / 2001 Semilente®, CSII with Humalog® since 8 / 2004, changing 2008
shortly to Apidra® + Insuman® Infusat and since 4 / 2010 Novorapid® - in summary: she got
porcine, human and all available analogue insulin sorts. Since about 2005 she progressively developed daily hyperglycaemia (up to ca. 400 – 600 mg/dl, independent from insulin dosages,
up to nearly 600 I.U. of insulin did not change anything) with several ketoacidosis comas, late postprandial severe hypoglycaemia with often hypoglycaemic comas mainly in the early
morning several times the week. HbA1c worsened from minimal 6.4 % to at last 10.3 % over
years (normal: 4.2 - 6.1%), not absolute uncommon in puberty.
She has been treated in some specialised diabetic institutions with several procedures
(educational programs, multiple injections therapy, CSII, CGMS, experimentally intravenous
therapy, underwent psychological and psychiatric explorations, family therapy) with no
ameliorating effect.
17 years old, she was referred to me with the question: Do you have any idea how to help her?
I could confirm the diagnosis of type-1-diabetes (C-peptide negative), but also found MODY-3-
genes and extreme amounts of insulin-antibodies (23 210 nU/mL, 81%-binding) and at first
extreme amounts of insulin-receptor-antibodies, but the latter seems to be a methodological
problem (free circulating IA-IRA-complexes). As “all” immune suppressive therapies failed
(glucocorticoids, azathioprin, mycophenolat3, Rituximab), first in case of urgent need (4
sessions in about 6 weeks) she is now precautionary constantly treated by immune adsorption
(reliable vascular access via Cimino-shunt similar to dialysis with a IgA-column, ADASorb®) 2
days a fortnight4. By extracting the IA-concentrations into the normal range, her total daily dose
sinks to about 50 I.U./ d /57 kg and her glucose metabolism stabilizes near normality, but her
antibody production persists. Now we wait if the I(A)As will decline - which has not happend the
last 2 years - and look for a definitely less invasive therapy, if possible, to avoid bone marrow
transplantation.
Abstract
Objective (aim): To collect IA-data status among T1D-patients in relation to their prior and
present used insulin sorts (compared with healthy persons, T2D- and MODY-patients)
Methods: Out of 291 consecutive participants from more than 4000 of my CSII-patients we
actually draw up 277 complete data sets of measured IA with two different methods (percentage
of binding and absolute amounts), last HbA1c and collected data belonging to their insulin
therapy.
Results: At a significance level p < 0,05 we found
- that significant more patients using analogue insulin produce IAs compared with human
insulin users,
- significant higher IA-levels in all T1D-patients compared with healthy persons,
- significant and / or borderline significant higher IA-levels in the group of analogue users
compared with human insulin users,
- in all cases significant higher IA-levels in the group of the aspart insulin users compared with
human-insulin users, users of the other analogue insulins and users of insulin derived from
animals.
Conclusion: The careless prescribing of insulin analogues must be reconsidered under these
results. It needs to be investigated urgently whether through the beginning of and the
conversion to the use of analogue insulins a dangerous development is provoked towards a
difficulty to control blood sugar metabolism as a result of IAs. All clinical diabetologists should
review and follow up their diabetics on their IA-status routinely.
Abbreviations
BMI (body mass index)
C-peptide (connecting peptide)
CSII (continuously subcutaneous insulin infusion = insulin pump treatment)
CGMS (continuous glucose monitoring system)
HbA1c (percentage of N-terminal glycated ß-chains of haemoglobin A1)
IA (insulin antibody)
IAA (insulin-auto-antibody)
ICT (intensified insulin therapy = multiple injections)
IgA (immunoglobulin class A)
i.U. (international Units)
m (male)
MODY (maturity onset diabetes in young people, here only type 2 and 3)
nU / mL (nano units per millilitre)
SD (standard deviation)
T1D (type-1-diabetes)
T2D (type-2-diabetes)
Introduction
Besides the rare insulinoma long be known, there is growing knowledge in the last years to the
rarer hyperinsulinaemic hypoglycaemia without insulinoma and not induced by artificial insulin
injection as insulin autoimmune syndrome (Hirata disease1,2) produced by insulin(receptor)-
antibodies in non-diabetic and type-2-diabetic persons5,6,7,8. Despite some methodological
problems9 there exists some knowledge of insulin antibodies as auto-antibodies of type-1-
diabetics10 (accompanying the ß-cell-destruction) and as acquired binding antibodies (even
allergic) provoked by insulin therapy itself in all diabetics. Purification of insulin in the 1970th
and the introduction of human insulin 1982 should and could reduce problems with bovine and
porcine insulin antibodies11. Recently there are reports to the higher levels of antibodies to
analogue insulin but without clinical opinion12,13.
Affected by the course of the disease of the above mentioned young woman, I found more
patients in my collective with similar although weaker but therapy relevant problems with high
insulin antibodies. Therefore I check all my patients routinely since October 2012 for IA for a
better understanding of metabolism problems. These are my alerting preliminary results – the
investigation will be extended and followed up.
Subjects, Materials and Methods
Participants:
From a cohort of 291 consecutive participants (13.10.12 – 24.1.13) we got 277 complete records:
245 T1D-patients (83 m), 241 on pump treatment,
2 within this group with additional MODY-Genes (2 m),
5 T2D-patients (4 m),
9 MODY-patients (6 m),
18 non diabetic persons (6 m) (= no insulin treatment)
|
Table 1: Characterisation of the participants |
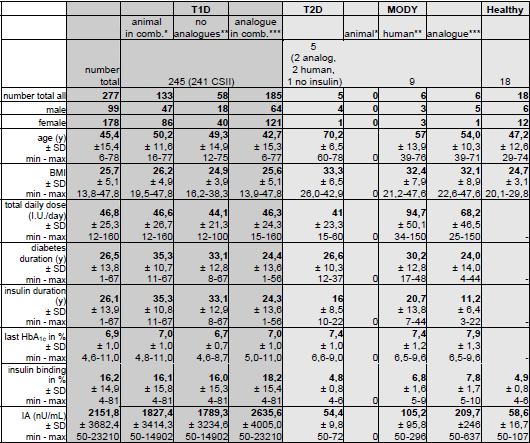
* all patients treated prior with animal derived insulins (porcine and bovine), 2 present with porcine, with possible
combination with other insulins, 37 without analogue contact (see Table 2)
** patients never treated with analogue insulins
***patients treated with analogues, possible contact with animal derived or human insulins |
Table 2: Patients using animal insulin without analogues (2 present with porcine insulin)
compared with patients using animal insulin and analogues too |

|
Measurements and data collection:
- Insulin antibodies absolute (nU/mL) performed by MVZ Labor PD Dr. Volkmann und Kollegen
GbR, Karlsruhe, Germany; [Normal range: < 110 nU/mL; gray zone: up to 250 nU/mL]
200 μL serum will be acidified with 250 μL 0,085M HCl, to dissociate immune complexes out of I(A)A und endogenous
insulin. Afterwards add 100 μL of a mixture of activated carbon, dextran and methylcellulose in buffer A (Na-phosphate buffer
with 0,33 M NaCl, 1,5% BSA), to bind endogenous insulin. After neutralization centrifuge the probes 10 min, 3750 x g. The
supernatant solution will be used in the further radio immune precipitation assay. 100 μL of the supernatant solution will be
diluted with 50 μL buffer A and 100 μL in buffer A diluted 125I-Insulin (PerkinElmer, Rodgau). Parallel replace 50 μL buffer A
by Insuman® rapid (Sanofi-Aventis, Frankfurt) for determination the unspecific binding of 125I-Insulin. After incubation the
probes overnight at 2-8°C, add 1,5 mL buffer B (0,1 M Tris-HCl, pH 8.0 with 17% PEG 6000). After further 20 min.
incubation at 2-8°C centrifuge the probes (30 min., 3750 x g,10°C). Add 1,5 mL buffer C (0,1 M Tris-HCl, pH 8.0 with 12,5%
PEG 6000) to the aspirated supernatant solution and mix it thoroughly. After 20 min. of incubation at 2-8°C centrifuge the
probes (30 min., 3750 x g, 10°C), aspirate the supernatant solution and measure the activity of the precipitated pellets in a
gamma-counter. The difference (activities of the precipitates of the specific and the unspecific test) will be converted into
nU/mL taking the date of calibration of 125I-Insulin into account.
The test result as nU/mL is an absolute quantity, specificity and cross reactivity unclear.
- Percentage insulin binding levels by radio-immunoassay product of DIAsource, formerly
BioSource, Belgium (AIA RIA kit, KIP0091) performed by Laboratory Limbach Heidelberg
Germany; [Normal range: < 10 %; borderline: 10 - 15 %]
The presence of circulating anti-insulin antibodies in patients treated with insulin will be assessed on a semi-quantitative
basis by the determination of the binding of 125I-Tyr-A14-insulin in the serum fraction by the polyethylene glycol (PEG)
(gammaglobulins) was precipitated. The used kit determined if the samples contain free anti-insulin antibodies, that
are not bound to the insulin. The concentration of insulin in the tracer is 0.42 nmol / 100 μl of tracer. The origin of insulin is
human recombinant with a purity > 99 % by HPLC ordered at Fitzgerald (USA). Item 1302129. The insulin is mono-iodated
on position A14 and purified by HPLC. Intra- and inter-assay CVs: 1,6-20% (lower CVs in higher IA-concentrations); Mean
of 80 healthy persons: 5,5 %; mean + 3 SD (= 8,2%): I(A)As positive.
This test does not measure the bound insulin in patients but in his serum in vitro under
special conditions. The test result as percentage of binding is a relative number and not an
absolute quantity, more than qualitative (antibody yes or no), less than quantitatively (=”semi
quantitative”), specificity and cross reactivity unclear.
- The HbA1c-measurements were mostly done with affinity chromatography (AfinionTM, product
of Axis-Shield PoC AS, Oslo, Norway), mostly performed by ourselves. [Normal range: < 6 %
(< 42,1 mmol/mol); coefficient of variation CV < 1,4%]
- Since October 2012 we extended our routine blood test for measuring the I(A)As in 2 different
laboratories in all T1D-patients of our CSII-courses and ambulatory. We routinely asked them
for their medical history. The data of age, gender, weight, height, diabetes duration, insulin
treatment duration, total daily dose, all previous and present insulin sorts and their application
duration, autoimmune state by the patients and their relatives, immune suppressive therapy
(present and past) and last HbA1c were filled in a questionnaire and in any doubt or obvious
contradiction in the questionnaire we checked stored data and made interviews, using if
necessary the services of medical reports. To control the details of the normal values of the
laboratories, we invited all healthy escorts of the T1D-patients, T2D-patients and ODYpatients
from our ambulatory to the same procedure.
- These data were transferred in an Excel data file (Microsoft®, table calculation program),
controlled by 2 persons and imported for statistical analyses into the statistic program Systat® 10.2 (www.systat.com), controlled by 3 persons, 2 of them are statistic professionals.
- As the data were not normal distributed we used the Mann–Whitney U test as a nonparametric
statistical hypothesis test for assessing whether one of two samples of
independent observations tends to have larger values than the other and the Kruskal–Wallis
one-way analysis of variance test by ranks for testing whether samples originate from the
same distribution, if we compare more than two samples. With Pearson X-squared test we
tested some null hypotheses. We define the limit for significance level to p = 0,05.
Descriptive statistics (mean values, standard deviations, correlations) were done by Excel,
non parametric tests were performed by Systat®.
Limitations, Possible Bias and Difficulties
For a better reminder, we gave our patients a list of about hundred historical and actual insulin
product names, additionally it was easier for the patients to recollect some insulin producing
companies, years of use and / or the origin of insulin. Therefore they could choose the origin of
insulin (bovine, porcine, human, analogue) or special information as importations or foreign
insulin. Many of the collected data were very precisely, p. e. reconstructed and confirmed by
medical prescriptions. Sometimes it was easier for the patients to remind for some insulin
producing companies, years of use and / or the origin of insulin – that enables reconstructions
too. The duration of application was more imprecise, yet you could depend on semi quantitative
results (shorter or longer than weeks, months, years). At all, we had to exclude only 4,8 % of
patients due to lack of reliable data.
We could not discriminate between insulin auto-antibodies and acquired antibodies and non
specificity due to cross reactivity between different insulin sorts. Though in average the
influence of IAAs in our patients should be much smaller than in children cohorts, as their mean
age was 45,4 years with an averaged diabetes duration of 26,5 years.
It is difficult to recruit “pure” groups of T1D-patients that use exclusively only one sort of insulin
over a longer time – and for the future nearly impossible. Before introduction of human insulin
about 30 years ago, they could have used only animal derived insulin (mostly bovine and
porcine, purified in the 1970th). The first analogue insulin starts about 17 years ago. So the
greatest majority has or has had contact with different sorts, different purities, different durations
and past periods. Nowadays, there is a growing group treated only with analogues – but we
have no peer group for comparison purposes. But we can form groups where one or some
sorts are missing and compare them to each other. IA derived from animals may persist for
more than 20 years11. |
Table 3: insulin usage groups in all of our patients |
 |
We selected our CSII-patients (241 of 245 T1D-patients) from our highly specialised institution
with the peculiarity that the influence of any long acting insulin, the analogues, too, stopped
mostly years ago totally.
As some of our significances failed sharply the 5 % level, we urgently need bigger groups. The
power of these data suffers from the high dispersion (high standard deviation) of the values. |
Results
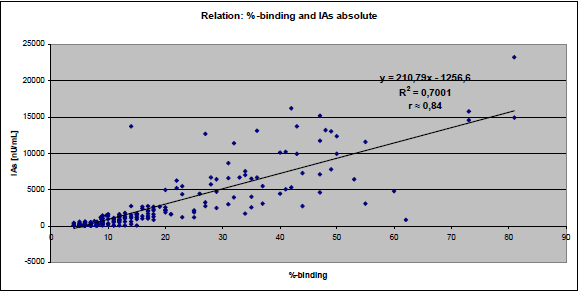
- Correlation between IA-binding and IA absolute is shown in the following figure. Repeated
measuring of some of the runaway values showed similar differences. Therefore each of the
compared methods have their specific problems, or they differ in what they are measuring.
Probably these differences also reflect the semi quantitative and the absolute method.
Figure 1: Relationship of the percentage of bound insulin to the absolute amount of insulin
antibodies [nU/mL] |
|
|
- Both IA-values for all healthy subjects were inside the normal ranges and confirmed these
normal ranges for our whole collective.
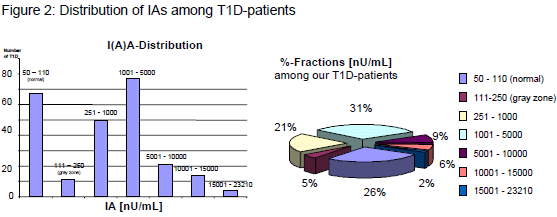
- We found significant higher IA-levels in all T1D-patients compared with healthy persons
(p < 0,000).
- 69 % of all T1D-patients exceed the IA normal range, 60 % the gray zone.
|
 |
- Significant more patients (almost twice as many) using analogue insulin produce IAs (p =
0,023; p = 0,04) compared with human insulin users,
- significant higher IA-levels in the group of analogue users compared with the rest of the
group (p < 0,05),
- borderline significant higher IA-levels in the group of analogue users compared with human
insulin users (p = 0,07),
- in all cases significant higher IA-levels in the group of the aspart insulin users compared with
human insulin users, users of the other analogue insulins and users of insulin derived from
animals (p = 0,003).
- The group of T2D- and MODY-patients is too small to make strong statements. Maybe, the
immunogenic impacts are less pronounced as rather an indication that autoimmune genes
also favour the IAs.
- There was no correlation between HbA1c and amount of IA due to the whole participants, but
the HbA1c-values of our problematic patients were higher.
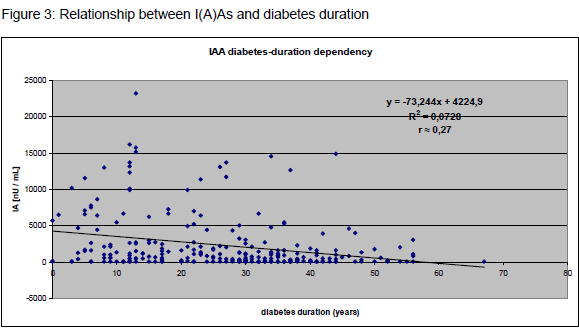
- It exists a weak correlation between I(A)As and diabetes-duration with a declining tendency
(see Figure 2). Other interesting correlations as to age, insulin and other autoimmune
diseases were too weak or not examinable due to weak data.
|
 |
Discussion and Conclusions
What is fact, what can we hypothesize? Animal derived insulin and also analogue insulin are not
produced naturally by the human body and all sorts are administered at unnatural routes.
Therefore the human immune system may detect and fend them off with humoral factors as it
does it with other foreign proteins, too.
We have measured significant larger different titers of IAs between T1D-patients treated with
short acting analogue insulin in contrast to T1D-patients treated with short acting human insulin
(may be only the effect of insulin aspart). First, no more, no less. We can further conclude from
our data that independent of high purity and origin, therapeutic insulins continue to be
immunogenic in humans. Finding antibodies is not a normal state, and the extent is surprising -
but it is initially only a laboratory and not (yet) a disease. We should ask: what do they matter?
We measured IAs with 2 different methods: %-binding of insulin and absolute concentrations of
IAs (nU/mL). In our data we see that they correlate indeed, but not very strongly (r ≈ 0,84). In
some persons there are big differences, therefore the methods have different problems or they
do not testify the same: when measuring percentage of binding-insulin there is always given
the same aliquot to patients serum samples independent from the patients insulin demand
(bigger differences in insulin sensitivity and need for eating and correction). But if we
understand well the clinical symptoms of hyperglycaemia when eating with administered insulin
and late postprandial hypoglycaemia as binding and releasing processes from the IA-buffer
(due to the law of mass action), then this process in vivo is much more dynamic and not
comparable with the % of bound insulin in vitro with constant insulin additive. If we look at
clinical consequences (hyperglycaemia – hypoglycaemia) this data seems less relevant. If we
want to describe the status of the IA-producing process, it is more reliable to determine absolute
amounts or concentrations of IAs.
Even if the frequency and the amount of IAs may be biased in our cohort by several factors (p.
e. nearly exclusive CSII-patients, no pure groups, high standard deviations,…), the
phenomenon of potentially life-threarening high titers of IAs exists as shown definitely in one of
them.
We see correlations and one is trying to take causalities. But we have to differentiate the first
period of time of type-1-diabetes with insulin-auto-antibodies (IAA): they may climb to high
values and may disappear relatively quickly and the possible parallel development later on or at
the same time with acquired insulin-antibodies (IA, which cannot surely be differentiated
specifically from the IAAs). But if there are significant differences between the frequency of the
occurrence due to sort and / or the amounts of I(A)As between human insulin and analogue
insulin, then at least these differences seem to be provoked by IAs.
Further on we see in our data that the more likely that T1D-patients were in contact with
analogues the higher are the titers in nU/mL: 1603,4 for treated with animal derived insulin,
without any contact to analogues - 1917 for animal derived insulin, with contact to analogues;
1789,3 no analogue contact - 2635,6 with analogue contact. In this sense we can break a
lance(t) for porcine insulin.
When on the one hand pediatricians see T1D-patients, then they look at the beginning of T1D
with different high titers of IAA. Maybe, in seldom cases they control them quantitatively when
they disappear, but naturally they have no good chance to see the development of acquired IAs
during the short period of the following part of the childhood. When on the other hand an
internal specialist sees T1D-patients, he then gets the T1D-patients sent from pediatricians, is
also visited by new diagnosed grown-up T1D-patients and sees the follow-up for decades in
both groups – and therefore he is confronted with the increasing / decreasing IAAs and the
increasing IAs. In a short period up to 2 years, Mianowska15 saw a climbing of the frequency of
semi quantitatively I(A)As from 80 % to 97.9 % with no difference between the insulin sorts– that is no proof that those children with T1D will not be in danger to develop acquired IAs sort
depending in bigger amounts later on. He sees this phenomenon as a consequence of the T1D
autoimmune process or the immunogenic consequences of insulin therapy that would disappear
spontaneously within 6 – 12 months. The diabetes duration of our problematic patients is much
longer than 12 months. We detect more than 10000 nU/ml I(A)As in 16 of our 245 T1D-patients
with diabetes duration longer than 10 years, in 8 longer than 20 years, in 3 longer than 30
years. Will they or some of them persist for a lifetime? This discussion remembered me on the
disastrous discussion in the past that children will not develop late-complications.
We have no data of the influence of the long-term analogue insulins to IAs. The most of our
patients never had and have contact with analogue long term insulin, or if so, only for a short
time or a long time ago.
Unfortunately, we cannot predict the course of the further development of IA, we have no follow
up yet. We assume that IAAs disappear more quickly and the acquired IAs will stay very long.
If we weigh human and anlogue short acting insulins due to the direct effect of bloodglucose
and the practicability in the everyday life, we see advantages and disadvantages for both insulin
sorts, likely in different patients and different life circumstances. Therefore, there is no need to
principally start with analogues concerning the therapy. It is too simple to call it the price of
modern therapy or modern lifestyle. But if you prescribe analogue insulin, you should inform the
patient to this risk and control their IA-status routinely. As we proclaim “empowerment” and “informed decision”, we should demand warning notices in the enclosed package insert of
insulin, if our findings should be confirmed.
Furthermore we should be more sensitive when we see daily long stretched hyperglycaemia
followed by late postprandial severe hypoglycaemia, especially in the early morning, and take in
consideration IA if bigger total daily dosages of insulin occur and should investigate future
surveillance of genesis and onset of acquired IA, their course and therapeutic impact.
When Fineberg16 et al summarize: “Little proof exists, however, that the development of insulin
antibodies (IAs) to exogenous insulin therapy affects integrated glucose control, insulin dose
requirements, and incidence of hypoglycaemia…” then Ishizuka T et al.14 is cited “encountered
two patients who developed daytime hyperglycaemia and early morning hypoglycaemia
because of insulin antibody (IA) that the affinity was extremely lower and the capacity extremely
higher than those of IA in the insulin autoimmune syndrome, after their insulin treatment were
changed from human insulin to analogue insulin.”
And I encountered a young patient with type-1-diabetes, who can only survive by continuous
immune adsorption therapy due to IA (maximum of 23210 nU/mL, 81-% binding) since more
than 2 years, likely caused by analogue insulin, but not by aspart insulin (because she only has
had contact with aspart insulin after the diagnosis of extreme I(A)A-values). At this extreme
endpoint, we can proof the life-threatening clinical impact of I(A)As. In this case, no standard
therapy exists. Nevertheless is there an analogy to the seldom autoimmune Hirata disease, first
described by Hirata et al. 1970. He reported a patient with insulin autoimmune syndrome,
followed 1994 by reports of 197 Japanese persons with the same disease1,2,5,6,8 and T2Dperson7,
now in T1D-patients?
But at least 3 further T1D-patients of my collective have bigger therapy-problems (daytime long
stretched hyperglycaemia, nocturnal severe hypoglycaemia) probably due to high IA-levels
(6373 nU/mL – 29 %; 16188 nU/mL – 42 %; 15178 nU/mL – 73 %) and some other patients with
similar quantitative combinations of nU/mL and % of IAs have obviously no therapy problems.
If the insulin-IA-associates have further negative aspects, we have even less informations.
I fear that we look only at the tip of the iceberg – or did I and my colleagues systematically
check our patients regarding to this phenomenon so far?
As an attempt to respond the title´s question, we have to extend it: Late revenge of analogue
insulins and/or footprints of T1D autoimmune process and/or unavoidable immunogenic
consequences of insulin therapy and/or Hirata-disease like among T1D-patients? Depending on
the patient we look at the beginning of T1D more to the footprints of autoimmune process and
later on more to unavoidable immunogenic consequences of insulin therapy, may be sometimes
an analogy to the seldom Hirata-disease (associated with HLADRB1*
0406/DQA1*0301/DQB1*0302?) – but we can not say exactly what of these options or
mixtures exist in the individual case – any way is particularly troubling that one or more
analogue insulin may play a triggering or reinforcing role. Now we can make mistakes in two
directions: Optimistic appeasing or panic mongering. We have more anxious questions and
should avoid a false sense of security. We should rather ask if there is an avalanche to come
on the long term? Does this phenomenon remain an exception or how often will it occur? We
should investigate it immediately – may be we have a chance to prevent it.
Acknowledgments
Dr. Jochen Selbach, nephrologist of Caritas Krankenhaus Bad Mergentheim, Germany
performed all immune adsorptions on our young T1D-patient.
Harald Schmidt, MVZ Labor Dr. Limbach and colleagues, performed all IA-measurements as
binding in %. He advised me on the laboratory method.
Dipl. Chem. Oliver Bauer of MVZ Labor PD Dr. Volkmann and colleagues GbR (Chief of the
autoimmune diagnostic department: Dr. Martin Blüthner) performed all IA-measurements as nU
/ mL and advised me on the laboratory method and described it in this article.
Kerstin Müller, Diabetes-Dorf Althausen, Bad Mergentheim, Germany took care of data
acquisition and data management.
Authors address, Conflict of interest
Dr. med. Bernhard Teupe, Diabetes-Dorf Althausen, Im Brunnental 10 – 18,
D-97980 Bad Mergentheim; Email: Teupe@DiabetesDorfAlthausen.de. No financial or advisory
connections to the insulin producing industry, no sponsoring from any side.
References
- Literature research by PUBMED.DE, DIMDI, Literature-Appendix at publications, spontaneous
Hirata Y; Uchigata Y: Insulin autoimmune syndrome in Japan. Diabetes research and
clinical practice 1994; 24 Suppl; p. S153-7
- Uchigata Y , Eguchi Y, Takayama-Hasumi S, Omori : Insulin autoimmune syndrome (Hirata
Disease): clinical features and epidemiology in Japan Review Article. Diabetes Research
and Clinical Practice 1994, 22, Issues 2–3, p89-94
- Segal, Allgrove et al.: Severe insulin resistance secondary to insulin antibodies: successful
treatment with immunsupressant MMF. Pediatric Diabetes 2008, 9, p. 250 - 254
- Koyama R; Nakanishi K; Kato M; Yamashita S; Kuwahara H; Katori H: Hypoglycemia and
hyperglycemia due to insulin antibodies against therapeutic human insulin: treatment with
double filtration plasmapheresis and prednisolone. The American journal of the medical
sciences 2005; 329 (5); p. 259-64
- Yeung CW; Mak CM; Lam KS; Tam S: Hypoglycaemia due to autoimmune insulin
syndrome in a 78-year-old Chinese man. British journal of biomedical science 2012; 69 (2);
p. 80-82
- Nasu T; Suzuki R; Okamoto Y; Miyata K; Uno A; Nakao R; Kawashima A; Nakao T; Kondo
M: Late postprandial hypoglycemia due to bioactive insulin dissociation from autoantibody
leading to unconsciousness in a patient with insulin autoimmune syndrome. Internal
medicine (Tokyo, Japan) 2011; 50 (4); p. 339-43
- Zhao TY; Li F; Xiong ZY: Frequent reoccurrence of hypoglycemia in a type 2 diabetic
patient with insulin antibodies. Molecular diagnosis & therapy 2010; 14 (4); p. 237-41
- Paiva ES; Pereira AE; Lombardi MT; Nishida SK; Tachibana TT; Ferrer C; Hauache OM;
Vieira JG; Reis AF: Insulin autoimmune syndrome (Hirata disease) as differential diagnosis
in patients with hyperinsulinemic hypoglycemia. Pancreas 2006; 32 (4); p. 431-2
- Kim S; Yun YM; Hur M; Moon HW; Kim JQ: The effects of anti-insulin antibodies and
crossreactivity with human recombinant insulin analogues in the E170 insulin
immunometric assay. The Korean journal of laboratory medicine 2011; 31 (1); p. 22-9
- Eisenbarth GS; Jeffrey J: The natural history of type 1A diabetes.
Arquivos brasileiros de endocrinologia e metabiologia 2008; 52 (2); p. 146-55
- Oak S; Phan TH; Gilliam LK; Hirsch IB; Hampe CS: Animal insulin therapy induces a
biased insulin antibody response that persists for years after introduction of human insulin.
Acta diabetologica 2010; 47 (2); p. 131-5
- Klingensmith GJ: Insulin antibodies - are they still with us? Do they matter? Pediatric
diabetes 2011; 12 (2); p. 75-7
- Chen JW; Frystyk J; Lauritzen T; Christiansen JS: Impact of insulin antibodies on insulin
aspart pharmacokinetics and pharmacodynamics after 12-week treatment with multiple
daily injections of biphasic insulin aspart 30 in patients with type 1 diabetes. European
journal of endocrinology / European Federation of Endocrine Societies 2005; 153 (6); p.
907-13
- Ishizuka T; Ogawa S; Mori T; Nako K; Nakamichi T; Oka Y; Ito S: Characteristics of the antibodies of two patients who developed daytime hyperglycemia and morning
hypoglycemia because of insulin antibodies. Diabetes research and clinical practice 2009;
84 (2); p. e21-3
- Mianowska B; Szadkowska A; Pietrzak I; Zmyslowska A; Wegner O; Tomczonek J;
Bodalski J; Mlynarski W: Immunogenicity of different brands of human insulin and rapidacting
insulin analogs in insulin-naive children with type 1 diabetes. Pediatric diabetes
2011; 12 (2); p. 78-84
- Fineberg SE; Kawabata TT; Finco-Kent D; Fountaine RJ; Finch GL; Krasner AS:
Immunological responses to exogenous insulin. Endocrine reviews (2007); 28 (6); p. 625-
|
Artikel als PDF
(PDF 178 KB)
|










